Implantation and the Decidua: How Your Body Prepares for the Placenta
Implantation and the Decidua: How Your Body Prepares for the Placenta
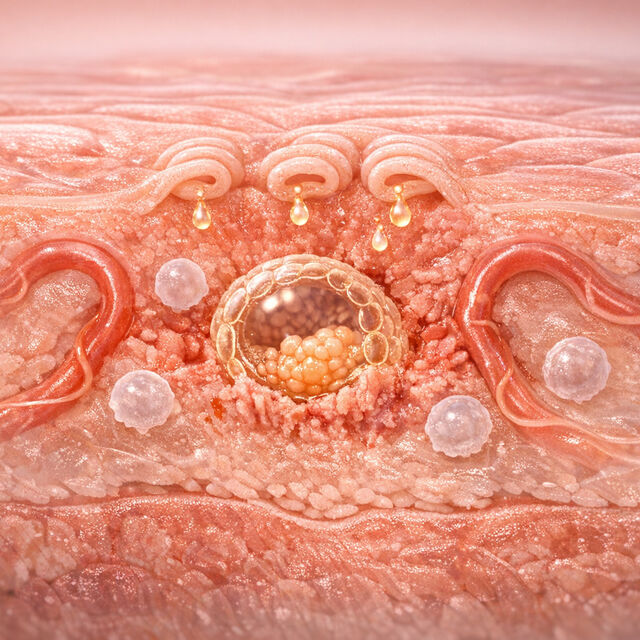
When pregnancy begins, your body undergoes a series of changes to support the development of a baby. Two critical processes in early pregnancy are implantation and the formation of the decidua. Implantation occurs when a fertilized egg, called a blastocyst, attaches to the uterine lining. The decidua is the transformed uterine lining that nourishes and protects the embryo while laying the groundwork for the placenta.
Here’s a quick breakdown of what happens:
- Implantation Timing: Occurs 5–9 days after fertilization during a short "window of implantation."
- Decidua Role: Provides nutrients, regulates immune responses, and supports hormonal changes.
- Placenta Formation: Begins with the decidua and ensures oxygen, nutrient exchange, and waste removal for the baby.
These processes ensure a stable environment for the embryo and prepare the uterus for the placenta, which sustains the baby throughout pregnancy. Proper timing, hormonal support, and immune regulation are key to a healthy start.
How Implantation Happens
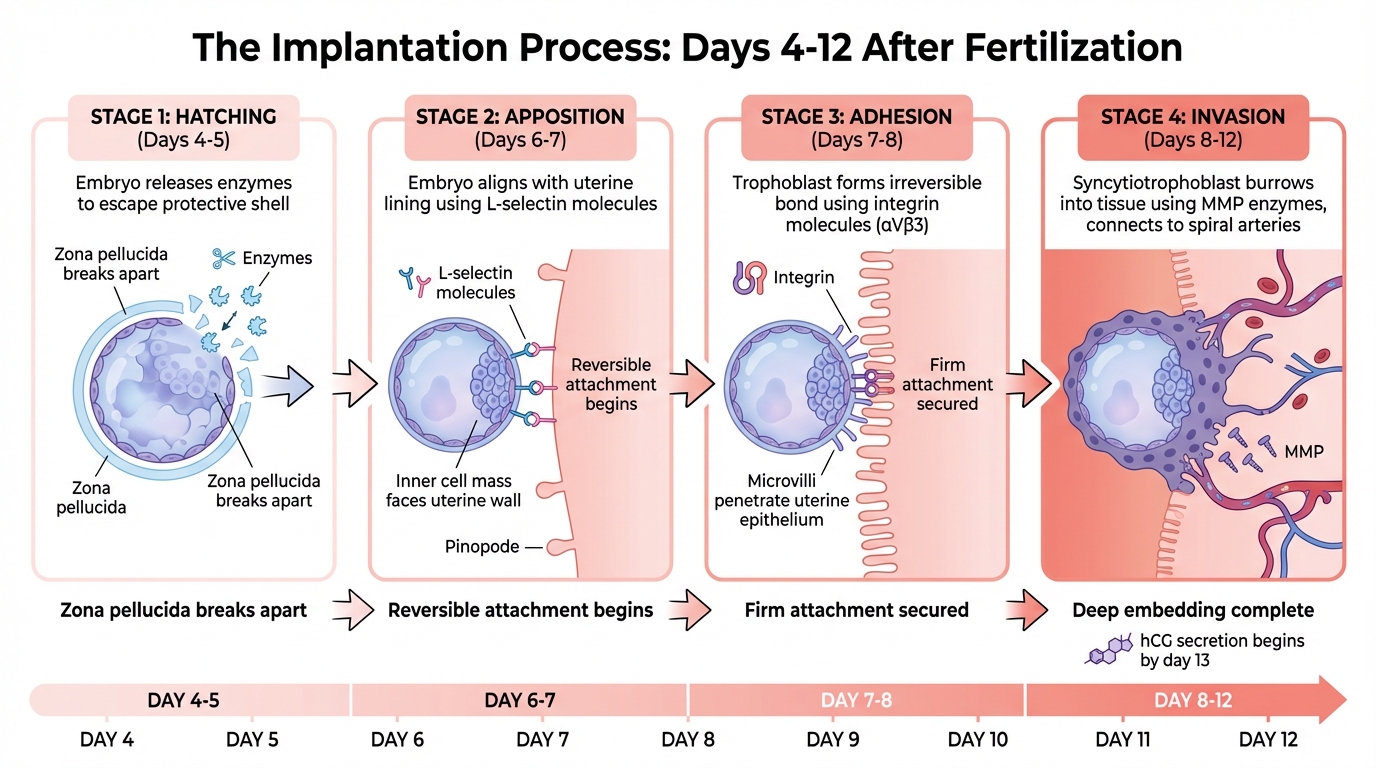
The 4 Stages of Embryo Implantation Timeline
Implantation is a step-by-step process that starts around days 5 to 9 after fertilization. During this time, the blastocyst - a hollow ball of cells - undergoes several changes. It breaks free from its protective shell, attaches to the uterine wall, and burrows into the tissue to connect with the maternal blood supply. These steps transform the embryo from a free-floating entity to one firmly embedded in the uterus.
Blastocyst Hatching and Positioning
The first step is for the blastocyst to escape its protective shell, the zona pellucida. This process, called zona hatching, typically occurs around days 4 to 5 after fertilization. The blastocyst releases enzymes that weaken and break apart this shell, allowing it to emerge and interact directly with the uterine lining.
Once free, the blastocyst begins the apposition phase, moving along the uterine lining to find the best spot for implantation. During this phase, the embryo aligns itself so that the inner cell mass - the group of cells destined to form the baby - faces the uterine wall. A molecule called L-selectin on the surface of the blastocyst acts like a tether, binding to structures known as pinopodes on the uterine lining. These pinopodes, which resemble tiny mushroom-shaped protrusions, appear during the implantation window (around days 20 to 21 of the menstrual cycle) and help draw the blastocyst closer by absorbing uterine fluid. At this stage, the connection is still reversible, but the embryo is preparing for the next step - embedding itself securely.
Trophoblast Invasion into the Uterine Lining
After apposition, the embryo moves into the adhesion phase (around days 7 to 8). During this stage, the blastocyst forms a stronger, irreversible bond with the uterine lining. The outer layer of the blastocyst, called the trophoblast, develops tiny projections known as microvilli that penetrate the uterine epithelium. This attachment is supported by molecules called integrins - specifically αVβ3 - that function like molecular Velcro. At the same time, the uterine lining removes proteins (MUC1 and MUC16) that normally prevent attachment, allowing the embryo to secure itself.
The process then transitions to invasion (days 8 to 12), where the embryo embeds deeply into the uterine tissue. The trophoblast splits into two layers: the inner cytotrophoblast and the outer syncytiotrophoblast. The syncytiotrophoblast, a continuous layer of fused cells, develops structures called invadopodia that actively burrow into the uterine tissue. These structures release enzymes, such as matrix metalloproteinases (MMP-2 and MMP-9), which break down the surrounding tissue and allow the embryo to integrate into the uterine stroma.
As the invasion progresses, the trophoblast reaches maternal blood vessels, specifically the spiral arteries, and remodels them into low-resistance channels. This ensures that the embryo receives a steady flow of maternal blood. By day 13 after fertilization, the wound at the entry site is sealed with a fibrin plug, and the syncytiotrophoblast begins secreting hCG (human chorionic gonadotropin), which supports progesterone production to maintain the pregnancy.
| Stage | Timing (Approx.) | Key Biological Action |
|---|---|---|
| Hatching | Days 4–5 post-fertilization | Blastocyst breaks free from the zona pellucida. |
| Apposition | Days 6–7 post-fertilization | Embryo loosely aligns with the uterine wall. |
| Adhesion | Days 7–8 post-fertilization | Firm attachment occurs; microvilli penetrate the epithelium. |
| Invasion | Days 8–12 post-fertilization | Syncytiotrophoblast embeds deeply and connects to blood vessels. |
sbb-itb-df90ce4
Decidualization: How the Uterus Prepares for Pregnancy
When a blastocyst implants, the uterine lining undergoes a process called decidualization, where the endometrium transforms into a specialized tissue known as the decidua. This transformation creates a nutrient-dense and immune-protected environment, crucial for supporting the embryo during the early stages before the placenta takes over.
What Triggers Decidualization?
The hormone progesterone, released by the corpus luteum after ovulation, is the primary driver of decidualization. Interestingly, in humans, this process begins spontaneously around day 22 of the menstrual cycle, even in the absence of pregnancy. Progesterone works alongside cyclic adenosine monophosphate (cAMP), a signaling molecule that prepares endometrial cells to respond effectively to the hormone.
"Decidualization of the human endometrium, which involves a dramatic morphological and functional differentiation of human endometrial stromal cells (ESCs), is essential for the establishment of a successful pregnancy." - Hidetaka Okada, Department of Obstetrics and Gynecology, Kansai Medical University
During this process, the spindle-shaped stromal fibroblasts in the uterine lining transform into large, rounded decidual cells. These cells stockpile glycogen and lipid droplets, providing essential nutrients for the developing embryo. They also produce specific proteins, such as decidual prolactin and insulin-like growth factor-binding protein 1 (IGFBP-1), which signal that the process is progressing as it should. Meanwhile, spiral arteries in the uterus remodel from high-resistance to low-resistance blood vessels, dramatically increasing uteroplacental blood flow - from about 50 mL/min before pregnancy to over 500 mL/min by the end of gestation.
The decidua also creates an immune-protected zone. It recruits specialized immune cells, particularly uterine natural killer (uNK) cells, that safeguard the embryo. These cells not only prevent the embryo from being rejected as foreign tissue but also assist in vascular remodeling. Additionally, the decidua carefully regulates the depth of trophoblast invasion, ensuring optimal placental attachment.
This complex transformation prepares the uterus both hormonally and nutritionally, while also organizing it into distinct layers with specialized functions.
The 3 Layers of the Decidua and Their Roles
After implantation, the decidua organizes into three layers, each with a unique function:
| Decidua Layer | Location | Primary Function |
|---|---|---|
| Decidua Basalis | Beneath the embryo implantation site | Forms the maternal side of the placenta, facilitating nutrient and gas exchange |
| Decidua Capsularis | Surrounds the embryo on the side facing the uterine cavity | Encloses the embryo and amniotic sac, eventually merging with the decidua parietalis as the pregnancy progresses |
| Decidua Parietalis (Vera) | Lines the rest of the uterine cavity | Provides structural support and fuses with the capsularis by weeks 12–16, closing the uterine cavity |
The decidua basalis plays a key role in placental development, acting as the interface for maternal and fetal tissue exchange. The decidua capsularis, initially covering the embryo like a protective cap, stretches as the fetus grows and the amniotic sac expands. By the fourth month, it merges with the decidua parietalis, which lines the rest of the uterus, ensuring structural support throughout pregnancy. Together, these layers form a carefully coordinated system that supports and sustains the growing fetus.
How the Decidua Leads to Placenta Formation
How the Placenta Develops from the Decidua
The decidua basalis, located beneath the implantation site, plays a crucial role in forming the maternal side of the placenta. It acts as the foundation where fetal trophoblast cells attach to create the placenta's structure. Together, these cells and the decidua form the fetomaternal junction, which facilitates the exchange of oxygen, nutrients, and waste between mother and fetus.
As trophoblast cells invade the decidua basalis, the decidua carefully regulates this process, ensuring proper attachment while preventing the cells from penetrating too deeply into the uterine muscle. A fibrinoid layer called Nitabuch's layer acts as a boundary to prevent excessive invasion, which could lead to complications like placenta accreta. Early in pregnancy, the decidua also provides histotrophic nutrition, supplying glucose, lipids, and growth factors through secretions from endometrial glands. This sustains the developing placenta until maternal blood flow is fully established.
Within the decidua basalis, spiral arteries undergo a significant transformation. Trophoblast cells replace the arterial lining, converting these narrow vessels into wide, low-resistance channels that support increased blood flow to the placenta. This remodeling, aided by uterine natural killer cells, boosts uterine blood flow by 10 to 12 times during pregnancy. Once the placental structure is in place, its role shifts to fully support fetal growth for the remainder of the pregnancy.
What the Placenta Does During Pregnancy
Once formed, the placenta resembles a spongy disc, about 8 inches across and 1.2 inches thick. It performs vital functions, all tied to its connection with the decidua. Maternal blood flows through remodeled spiral arteries into the placental villi, where nutrients like glucose, amino acids, and vitamins are transferred to the fetus, while waste products such as urea, uric acid, and bilirubin are removed.
The placenta also acts as an endocrine organ, producing hormones critical for pregnancy. It secretes human chorionic gonadotropin (hCG), which supports progesterone production to maintain the decidua. Other hormones like estrogen and placental lactogen are also produced, playing roles in sustaining pregnancy and preparing the body for breastfeeding. The decidua’s immune-regulatory functions further ensure immune tolerance, creating an environment that supports the baby's growth from the earliest stages until birth.
Conclusion: The Natural Process of Early Pregnancy
Implantation and decidualization are key steps in laying the groundwork for a healthy pregnancy. During this time, the embryo secures itself to the uterine wall, while the decidua transforms the uterine lining into a nutrient-rich area. This process not only regulates trophoblast invasion and remodels spiral arteries to boost blood flow but also establishes immune tolerance to safeguard the embryo. These intricate changes ultimately pave the way for placenta formation, which will sustain your baby throughout the pregnancy.
"Proper development of the placenta is essential for a successful pregnancy." - Elizabeth J. Herrick and Bruno Bordoni, StatPearls
The placenta plays a critical role in pregnancy success. Understanding how your body prepares during these early stages can offer a deeper appreciation for the complex biological processes happening behind the scenes.
In addition to these natural events, maintaining a nutrient-rich diet - especially one high in zinc - can support healthy blastocyst development. Avoiding smoking and effectively managing chronic conditions like hypertension or diabetes can also contribute to better placental health and lower the risk of complications.
If you have concerns about early pregnancy symptoms, a history of miscarriage, or questions about placental health, reach out to your healthcare provider. They can offer tailored advice and monitor your pregnancy to help ensure both you and your baby stay healthy in the months to come.
FAQs
What are the earliest signs that implantation happened?
The first hints of implantation might include light spotting (often called implantation bleeding), mild cramping, and subtle shifts in basal body temperature. These symptoms usually show up 6 to 12 days after ovulation. However, it’s worth noting that these signs can differ from person to person, and some may not notice them at all.
How does the decidua stop my immune system from rejecting the embryo?
The decidua is a unique tissue in the uterus that plays a key role in ensuring the immune system doesn’t reject the embryo. It achieves this by creating an environment that encourages immune tolerance. One way it does this is by releasing molecules that help regulate immune responses. Additionally, it promotes regulatory T (Treg) cells, which work to suppress any immune reactions that could target the fetus.
Specialized immune cells, such as uterine natural killer (uNK) cells and macrophages, also adjust their behavior to support the pregnancy. While they help protect against infections, they ensure the embryo remains unharmed, striking a delicate balance between defense and tolerance.
What can go wrong if the placenta forms or attaches abnormally?
Abnormal placental attachment, including conditions like placenta accreta, increta, or percreta, can result in severe bleeding during childbirth, posing serious risks to both mother and baby. These issues may also lead to placental abruption, where the placenta detaches too early. This can cause fetal distress or even miscarriage. Furthermore, when the placenta doesn't develop properly, it can limit the exchange of nutrients and oxygen, which may hinder fetal growth and raise the likelihood of complications such as preeclampsia.
The views, statements, and pricing expressed are deemed reliable as of the published date. Articles may not reflect current pricing, offerings, or recent innovations.