IVF Day 3 Crash: Paternal DNA & Cannabis
The "Day 3 crash" in IVF refers to embryos halting development at a critical stage, often due to genetic or environmental factors. This stage is when the embryo switches from maternal to its own genetic programming, known as embryonic genome activation (EGA).
Key takeaways:
- Paternal DNA quality plays a significant role after Day 3. DNA fragmentation in sperm can disrupt embryo development, even if early stages seem normal.
- Cannabis use by men has been linked to altered sperm DNA and lower IVF success rates. THC can impact sperm function and epigenetic patterns, increasing risks of embryo arrest.
- Solutions include sperm DNA testing, lifestyle changes (avoiding cannabis, alcohol, and tobacco), and medical interventions to improve sperm quality. Abstaining from cannabis for at least six months before IVF is recommended.
Understanding these factors and taking proactive steps can improve IVF outcomes and support healthier embryo development.
How Paternal DNA Quality Affects Embryo Development
After Day 3, when the embryo activates its own genome, compromised paternal DNA can cause the embryo to arrest.
DNA Fragmentation in Sperm and Embryo Arrest
DNA fragmentation refers to breaks or damage in the genetic material carried by sperm. This type of damage can disrupt embryo development during the critical stage of genome activation.
Paternal DNA damage has been closely tied to Day 3 embryo arrest. Even if early development seems normal, fragmented DNA or altered epigenetic patterns - chemical markers that regulate gene expression - can halt progress once the embryo starts relying on its own genome. For example, studies have shown that genes like DLGAP2 exhibit altered methylation in sperm from regular cannabis users. These epigenetic changes can directly impact whether an embryo continues to grow or arrests.
"The more cautious conclusion is that cannabis-related sperm changes and DNA fragmentation offer a plausible mechanism that could contribute to embryo arrest." - Staff Consortium
One key issue is that standard semen analysis - used to evaluate sperm count, motility, and shape - does not measure DNA integrity. This means a man can have a "normal" semen analysis but still carry significant DNA damage that negatively impacts IVF outcomes.
To address this, specialized tests are available to assess sperm DNA integrity more accurately.
Testing Options for Paternal DNA Quality
Advanced testing methods now make it possible to measure sperm DNA fragmentation, providing critical insights for IVF treatment. If you're dealing with unexplained infertility or recurrent embryo arrest, these tests can help identify underlying issues. Here are some commonly used assays for assessing sperm DNA integrity:
| Test Method | What It Measures | Key Benefit |
|---|---|---|
| SCSA (Sperm Chromatin Structure Assay) | Susceptibility of DNA to acid-induced damage | Standardized with clear thresholds for results |
| TUNEL | Directly measures DNA strand breaks | Identifies physical damage in individual sperm cells |
| Comet Assay | DNA migration patterns under electrophoresis | Extremely sensitive, detecting even low levels of damage |
| SCD (Sperm Chromatin Dispersion) | Presence or absence of DNA halos | Quick and simple, requiring minimal equipment |
These tests produce a DNA Fragmentation Index (DFI), which indicates the percentage of sperm with damaged DNA. Modern automated imaging platforms now use machine learning to analyze individual sperm, reducing human error and improving accuracy.
If elevated DNA fragmentation is detected, fertility specialists can recommend tailored solutions. Options may include lifestyle changes or advanced sperm selection techniques, such as microfluidic sorting or magnetic-activated cell sorting (MACS), to improve the quality of sperm used during fertilization.
Cannabis Use and Sperm Health
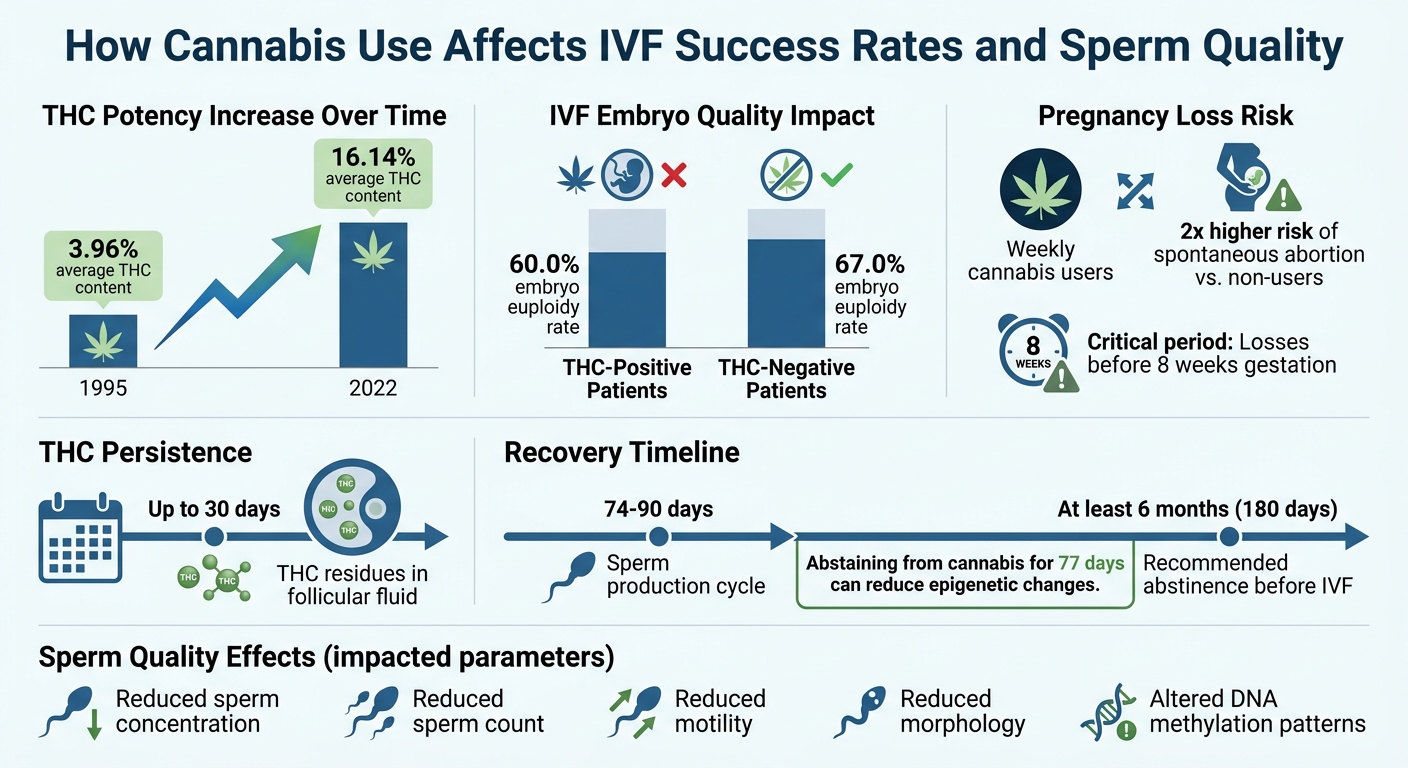
Lifestyle choices, such as cannabis use, can significantly impact sperm quality and, in turn, early embryo development. As cannabis use becomes more common among reproductive-age individuals, research highlights its negative effects on sperm health. The psychoactive compound in cannabis, THC, not only affects brain function but also disrupts sperm function. It activates CB1 and CB2 receptors in the male reproductive system, throwing off the balance required for healthy sperm.
How Cannabis Affects Sperm Quality
THC has been shown to reduce sperm concentration, count, motility, and morphology - essential factors for successful fertilization. But the impact goes deeper than what standard semen analysis can detect.
THC interferes with mitochondrial function in sperm, which is crucial for movement and the acrosome reaction (the process that allows sperm to penetrate an egg). By activating the CB1 receptor, THC can cause premature capacitation, essentially exhausting the sperm before it reaches the egg.
"Phytocannabinoid exposure to sperm may adversely affect sperm function by stimulating premature capacitation. These findings also show for the first time that spermatozoal transcripts may be altered by THC exposure." - BMC Molecular and Cell Biology
Additionally, regular cannabis use can alter DNA methylation patterns in sperm. These changes may disrupt embryonic genome activation around Day 3, increasing the risk of embryo arrest. Such cellular-level disruptions can have serious implications for IVF outcomes.
Cannabis Use and IVF Outcomes
Research consistently links paternal cannabis use to poorer IVF results. One study involving 1,535 couples found that men who used marijuana at least once a week had about twice the risk of spontaneous abortion compared to non-users. This association held even when the female partner did not use cannabis, emphasizing the significant role of paternal factors in early pregnancy loss.
The timing of pregnancy loss is particularly telling. The strongest link was observed in losses occurring before 8 weeks, a critical period when embryonic development heavily depends on genetic input from both parents. THC-induced changes in sperm transcripts may lead to developmental issues during genome activation, potentially causing the so-called "Day 3 Crash" often seen in IVF cycles.
"We don't know whether they [epigenetic changes] are going to be permanent. I would say, as a precaution, stop using cannabis for at least six months before trying to conceive." - Dr. Susan Murphy, Researcher, Duke University
There’s some good news, though. A 2021 Duke University study revealed that abstaining from cannabis for 77 days - approximately one full sperm production cycle - can reduce many of these epigenetic changes. However, since some effects may linger, experts recommend avoiding cannabis for at least six months before trying to conceive or beginning an IVF cycle.
These findings highlight the importance of addressing paternal lifestyle choices to support healthy embryo development during IVF.
How to Improve Paternal Factors for IVF Success
Research shows that paternal DNA integrity and lifestyle choices play a big role in embryo quality. By focusing on improving these factors, men can directly influence the success of an IVF cycle.
Taking steps to optimize health ahead of time is crucial. Many factors are within your control, and even small adjustments can make a difference in the months leading up to IVF.
Lifestyle Changes to Improve Sperm Quality
The 90 days before starting IVF is a critical time for making changes. This period aligns with a full sperm production cycle (roughly 74 to 90 days), so the sperm produced three months later will reflect the improvements made now.
One of the most important changes? Stop using cannabis at least six months before beginning IVF. Cannabis use has been shown to significantly harm sperm quality. Abstaining for a full sperm production cycle can reduce potential epigenetic effects. As Dr. Susan Murphy from Duke University explains:
"We don't know whether they are going to be permanent. I would say, as a precaution, stop using cannabis for at least six months before trying to conceive."
Beyond cannabis, cutting back on alcohol and tobacco is also key. Excessive alcohol can damage testicular tissue and disrupt hormones, while nicotine harms semen quality in a dose-dependent way. If you're using opioids, talk to your doctor about alternatives, as these can impair sperm production as well.
During this three-month window, focus on improving sleep, maintaining a healthy diet, exercising regularly, and managing stress. These habits help create the ideal environment for producing healthy sperm.
If lifestyle changes alone aren’t enough, medical treatments may provide additional support.
Medical Treatments for Paternal DNA Problems
If you’ve experienced repeated embryo arrest or poor fertilization rates, ask your doctor about sperm DNA fragmentation testing. This test goes deeper than a standard semen analysis by examining the genetic integrity of sperm.
Antioxidant supplements, such as Vitamin C and Melatonin, may also help reduce oxidative stress, which can harm testicular function. However, always consult with your reproductive endocrinologist before starting any supplements to ensure they’re safe and effective for your situation.
It’s also important to be open with your fertility team about any history of substance use, including cannabis, alcohol, or tobacco. This transparency helps them create a treatment plan tailored to your needs and set realistic expectations. If you’ve been trying to conceive for over a year without success - or for six months if your partner is over 35 - consider a full fertility evaluation.
For couples pursuing IVF, these changes go beyond simple lifestyle advice. With each IVF cycle costing between $15,000 and $20,000 and carrying emotional challenges, optimizing paternal factors is not just helpful - it’s essential.
Newborn Stem Cell Banking for IVF Families
In addition to improving sperm quality, taking steps to secure biological resources at birth can play a crucial role in protecting your child’s future health.
For IVF families dealing with challenges like embryo arrest or compromised paternal factors, stem cell banking acts as a form of biological safety net. It complements efforts to boost embryo viability by providing a backup plan for potential health issues that may arise later in life.
How Stem Cell Banking Supports IVF Families
IVF families often face distinct challenges that make stem cell banking an appealing option. For instance, paternal cannabis use has been linked to changes in DNA methylation in sperm, impacting vital developmental genes like DLGAP2. Research also shows that THC-positive IVF patients have a lower embryo euploidy rate - 60.0% compared to 67.0% in THC-negative patients.
By banking cord blood, cord tissue, and placental tissue, families can secure high-quality stem cells that may be used in future regenerative treatments. For those who experienced embryo arrest or reduced euploidy rates during their IVF journey, this proactive step provides long-term health security for their child.
Additionally, THC residues in follicular fluid can linger for up to 30 days, underscoring the importance of taking early precautions like stem cell banking. With the average THC content in cannabis increasing from 3.96% in 1995 to 16.14% in 2022, the potential impact on reproduction has grown considerably.
Americord Registry's Complete Family Plan
Americord Registry provides a comprehensive solution for families looking to capitalize on these benefits. Their Complete Family Plan includes banking for cord blood, cord tissue, and placental tissue, all processed using CryoMaxx™ technology and stored in 5-compartment vials, offering maximum flexibility for future use.
For IVF families, this plan ensures robust protection. Each type of stem cell has unique regenerative properties, giving your child access to a range of treatment possibilities as advancements in medical science continue. With clear pricing and dedicated support, Americord simplifies the process of securing this vital biological safety net at the time of birth.
Conclusion: Key Points for IVF Success
The quality of paternal DNA and cannabis use play a critical role in embryo viability, especially during the Day 3 transition when paternal DNA activation occurs. Research highlights that DNA fragmentation in sperm and cannabis use can significantly impact embryo development during this stage.
Evidence suggests that preconception cannabis use increases the likelihood of pregnancy loss and negative infant outcomes. However, discontinuing cannabis use may help reverse some of these effects. Considering that men of reproductive age have the highest global rates of substance use, addressing this issue is crucial for couples undergoing IVF.
For those pursuing IVF, focusing on paternal health is essential. Steps like consulting a healthcare provider, eliminating cannabis and heavy alcohol use, and exploring DNA fragmentation testing can lead to improved semen quality and lower the risk of pregnancy loss. These changes not only enhance IVF success but also contribute to the long-term health of the child.
Additionally, safeguarding biological resources through newborn stem cell banking provides an extra layer of security for your child’s future health. For families who have faced challenges like embryo arrest, Americord Registry’s Complete Family Plan offers a solution. This plan enables the storage of cord blood, cord tissue, and placental tissue using CryoMaxx™ technology, ensuring flexibility for future medical needs.
FAQs
How do I know if sperm DNA fragmentation is causing a Day 3 crash?
Testing for sperm DNA damage can provide insights into whether DNA fragmentation might be playing a role in a Day 3 crash. Elevated levels of DNA fragmentation have been associated with poor reproductive outcomes, such as embryo arrest during this crucial stage of development. It's worth discussing testing options with your fertility specialist to gain a clearer picture of how this factor could be affecting embryo development.
How long should men stop using cannabis before IVF?
Men planning for IVF should avoid cannabis use for at least three months before the procedure. This timeframe helps lower the risk of sperm undergoing epigenetic changes, which have been associated with early pregnancy loss tied to paternal cannabis consumption. Steering clear of cannabis during this period can promote healthier sperm and better support embryo development.
What can we do if sperm DNA fragmentation is high?
Improving sperm DNA fragmentation often starts with lifestyle changes. Reducing exposure to toxins, quitting smoking, and cutting back on alcohol can make a difference. Fertility specialists might also suggest advanced reproductive techniques like ICSI (Intracytoplasmic Sperm Injection), which can work around DNA damage in sperm. Additionally, antioxidant therapy may help lower oxidative stress, though its success can vary from person to person.
For a tailored approach, it's best to consult a fertility expert. They can guide you through lifestyle adjustments or medical treatments designed to boost sperm quality and improve the chances of a successful IVF outcome.
The views, statements, and pricing expressed are deemed reliable as of the published date. Articles may not reflect current pricing, offerings, or recent innovations.




