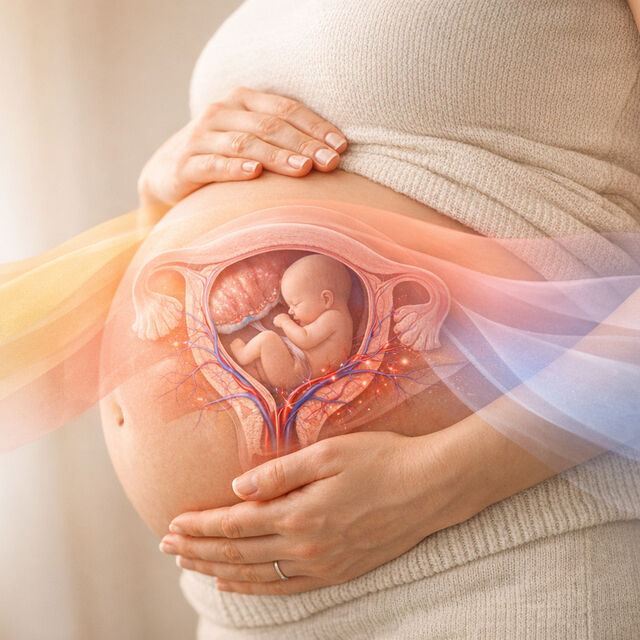
How Hormones Transform the Uterus to Support Your Baby
During pregnancy, your body undergoes incredible changes, driven by hormones like hCG, progesterone, estrogen, and relaxin. These hormones prepare your uterus to support a growing baby by:
- hCG: Signals the body to produce progesterone, maintains the uterine lining, and calms uterine muscles to protect the embryo.
- Progesterone: Thickens the uterine lining, promotes blood vessel growth, and keeps muscles relaxed to prevent early contractions.
- Estrogen: Enlarges the uterus, boosts blood flow, and supports tissue growth for a healthy pregnancy.
- Relaxin: Softens pelvic ligaments and cervix, preparing the body for childbirth.
hCG: The First Pregnancy Hormone
Human chorionic gonadotropin, or hCG, is the very first hormone your body produces after conception. Often referred to as the "pregnancy hormone", it’s made by cells in the developing placenta shortly after a fertilized egg implants in your uterus - usually around 10 days after fertilization. This is the hormone that pregnancy tests pick up in your blood or urine, with levels over 25 mIU/mL typically confirming pregnancy.
What’s fascinating about hCG is how fast it increases. During the first eight to 10 weeks, hCG levels nearly double every two to three days. They start at around 5–50 mIU/mL at three weeks and can reach up to 288,000 mIU/mL by weeks nine to 12. This rapid rise signals your body to prepare the uterus for the growing embryo.
How hCG Supports Progesterone Production
One of hCG’s key roles is to keep the corpus luteum - a temporary structure in the ovary - functioning. Normally, the corpus luteum would break down about two weeks after ovulation if pregnancy didn’t occur. But hCG steps in to maintain it, ensuring it continues to produce progesterone during the early weeks of pregnancy.
Think of hCG as a more powerful version of luteinizing hormone (LH). Both hormones bind to the same receptors, but hCG has a much longer half-life - around 37 hours compared to LH’s 25–30 minutes. This allows hCG to provide steady, continuous support. For about three to four weeks after implantation, hCG-driven progesterone production sustains the uterine lining until the placenta is ready to take over, typically between weeks seven and nine.
Relaxing the Uterus in Early Pregnancy
Beyond its role in progesterone production, hCG also helps calm your uterine muscles. It suppresses myometrial contractions, which are the muscle movements that could disrupt implantation or early embryo development. This creates what experts call a "quiet uterine environment", giving the embryo the stability it needs to attach and begin forming the placenta.
"The actions of hCG allow a coordinated growth of the fetus and uterus, signal the endometrium of impending implantation, support the growth and differentiation of the umbilical cord, and promote fetal growth and organogenesis." - StatPearls
hCG also encourages the growth of new blood vessels in the uterine wall and dilates spiral arteries, reducing resistance and ensuring plenty of blood reaches the developing placenta. Together with other hormones, hCG helps set the stage for the significant uterine changes needed to support your baby during these critical early weeks.
Up next, we’ll dive into how progesterone further prepares the uterus for a healthy pregnancy.
Progesterone: Preparing the Uterine Lining
After hCG gets things started, progesterone steps in to fine-tune the uterine environment, ensuring it's ready to support a pregnancy. Initially produced by the corpus luteum and later by the placenta (starting around week 7), progesterone drives some of the most crucial changes in the uterus during pregnancy.
"Progesterone is considered the most important steroid product... because progesterone alone can maintain a pregnancy that would otherwise abort." - Reshef Tal, MD, PhD, and Hugh S. Taylor, MD, Yale School of Medicine
Thickening the Uterine Lining and Boosting Blood Flow
One of progesterone's primary roles is transforming the uterine lining into a nutrient-rich, supportive environment. This process, known as secretory transformation, begins during the luteal phase and continues into early pregnancy. The lining undergoes decidualization, where regular endometrial cells change into specialized decidual cells packed with glycogen and lipids. These nutrients are essential for the embryo as it implants and starts to grow.
Progesterone also stimulates a surge in blood vessel development. It promotes the production of angiogenic factors like VEGF, bFGF, and TGF-β, which help form spiral arteries and increase capillary density. This expanded vascular network is critical - uterine blood flow increases more than 40-fold during pregnancy to supply oxygen and nutrients to the baby while removing waste. Beyond preparing the lining, progesterone also readies the uterus for significant growth.
Supporting Uterine Expansion
Progesterone plays a key role in keeping the uterus relaxed and adaptable throughout pregnancy. While hCG starts the process of muscle relaxation, progesterone ensures it continues by activating genes that suppress labor-related proteins like the oxytocin receptor and Connexin 43. It also boosts potassium channel expression, reducing uterine muscle activity and preventing premature contractions.
This relaxation is vital as the uterus stretches to accommodate the growing baby. Progesterone also reduces vascular resistance in the uterine walls, allowing them to expand easily while maintaining increased blood flow. In fact, total systemic vascular resistance decreases by 20% during pregnancy, thanks in large part to progesterone's vasodilatory effects. These changes create the space and flexibility needed for the baby to grow safely over the months ahead.
Estrogen: Supporting Uterine Growth and Circulation
While progesterone ensures the uterine lining is prepared and the muscles remain relaxed, estrogen plays a vital role in expanding the uterus and improving its circulation. By the time of childbirth, estrogen levels rise 30-fold, driving uterine growth and boosting blood flow to sustain your baby’s development.
Enlarging the Uterus and Supporting Tissues
Estrogen helps the uterus grow to nearly 20 times its original size during pregnancy through two key mechanisms. First, it causes hypertrophy, which enlarges the existing uterine cells. Second, it triggers hyperplasia, creating new cells. Together, these processes provide the necessary space for your baby to grow over the nine months.
In addition to enlarging the uterus, estrogen promotes the formation of new blood vessels within the uterine wall. It achieves this by increasing the activity of growth factors such as VEGF (Vascular Endothelial Growth Factor), bFGF, and TGF-β, which signal the creation of capillaries and arterioles. Estrogen also activates enzymes like MMP-2 and MMP-9, which remodel and break down the extracellular matrix to support vascular growth.
Increasing Blood Flow to the Uterus
This uterine growth sets the stage for a dramatic increase in blood flow. During pregnancy, blood flow to the uterus increases more than 40-fold, rising from less than 1% of your cardiac output to as much as 25% by the end of gestation. Estrogen is responsible for roughly 60% to 70% of this surge.
"Pregnancy is a physiological state that involves a significant decrease in uterine vascular tone and an increase in uterine blood flow, which is mediated in part by steroid hormones, including estrogen." - Katherine Chang, BS, Center for Perinatal Biology
Estrogen works as a powerful vasodilator. It enhances nitric oxide production by upregulating eNOS, activates BKCa channels in vascular smooth muscle, and reduces myogenic tone - the natural tendency of arteries to constrict. The radius of uterine arterioles increases about 10-fold during pregnancy. According to Poiseuille's law, this widening significantly boosts blood flow through these vessels, ensuring the growing baby receives the nutrients and oxygen it needs.
Additional Hormones That Support the Uterus
How Relaxin Prepares the Pelvis and Cervix
While estrogen and progesterone handle much of the work during pregnancy, relaxin plays an important role in getting your body ready for childbirth. This hormone, first produced by the corpus luteum and later by the placenta, reaches its highest levels around 12 to 14 weeks of pregnancy. It then decreases before rising again just before delivery.
Relaxin's key function is to make your pelvic area more flexible. It softens the ligaments, especially at the symphysis pubis, allowing the pelvis to widen so your baby can pass through the birth canal. It also helps your cervix prepare for labor by softening, lengthening, and widening it. For a vaginal birth, the cervix needs to dilate to 10 cm.
"In preparation for childbirth, it relaxes the ligaments in the pelvis and softens and widens the cervix." - Society for Endocrinology
Relaxin doesn’t stop at the pelvis and cervix. It also helps relax blood vessels to handle the 30% increase in blood volume (about 1 to 2 liters) that occurs during pregnancy. This ensures better blood flow to both the placenta and kidneys. However, this hormone’s effects on ligaments and joints throughout the body can leave you feeling a bit unsteady. Using supportive measures can help manage any discomfort. All these changes, guided by relaxin and other hormones, work together to prepare your body for labor and delivery.
How Hormones Work Together
Pregnancy is a team effort when it comes to hormones. While hCG, progesterone, and estrogen take center stage, hormones like relaxin fine-tune the process. Relaxin and progesterone work hand in hand - relaxin supports the structural and vascular changes that complement progesterone’s role in keeping uterine muscles relaxed.
As pregnancy advances, the balance between estrogen and progesterone becomes increasingly important. Estrogen promotes uterine growth and boosts blood flow, while progesterone maintains a calm uterine environment by suppressing contractions. Toward the end of pregnancy, this balance shifts. Progesterone levels level off, while estrogen continues to rise, making the uterine muscles more responsive to signals that trigger labor. Meanwhile, hCG, produced by the placenta, ensures the continued production of both relaxin and progesterone, helping all these hormones work together to support your baby’s growth and prepare your body for birth. This intricate hormonal coordination helps your body adapt to the many changes of pregnancy.
Managing Physical Changes During Pregnancy
Keeping track of how your uterus grows and how your circulation changes can give you a better understanding of the physical effects of pregnancy hormones. These measurements and symptoms provide a tangible connection between the hormonal shifts happening inside and how they show up in daily life.
Tracking Uterine Growth and Circulation
At every prenatal visit, your healthcare provider will measure your fundal height. Starting around the 20th week of pregnancy, this measurement in centimeters usually aligns with the number of weeks you’re pregnant (e.g., 24 cm at 24 weeks), with a normal range of about 2 centimeters above or below. Certified Nurse-Midwife Ellen Smead explains:
"What we want to look for is abnormally small or large measurements, and also if uterine measurement is consistent over time."
The uterus undergoes dramatic growth during pregnancy. By 12 weeks, it’s about the size of a grapefruit. By 20 weeks, it reaches your belly button, and by 36–40 weeks, it stretches from the pubic bone to the ribcage. Its weight also increases significantly - from about 1 ounce (50–60 grams) to around 2 pounds (900–1,100 grams) by the time of delivery.
Your blood volume also increases by 30%–50% (roughly 1–2 liters) to support your baby and the placenta. This extra blood flow may result in the "pregnancy glow" or mild swelling in your hands and feet. However, if you notice excessive swelling in your legs, severe headaches, or reduced fetal movement, contact your provider right away - these could point to circulation issues.
As your body adapts, you’ll likely experience physical symptoms that shift with each trimester.
Handling Common Symptoms by Trimester
These physical symptoms are closely tied to the hormonal adjustments your body makes throughout pregnancy.
Second trimester symptoms often stem from the hormone relaxin, which loosens pelvic ligaments and joints. To stay comfortable, wear supportive shoes and avoid sudden movements to keep your balance steady. Mild cramping or practice contractions (Braxton Hicks) may also occur. Resting and staying hydrated can usually help ease these sensations.
Third trimester symptoms tend to be more pronounced as your uterus reaches its largest size. Swelling in your feet and ankles is common due to increased estrogen and blood volume. To manage this, elevate your feet when resting and try gentle activities like walking or swimming to improve circulation. For heartburn caused by progesterone relaxing the esophageal sphincter, eat smaller, more frequent meals and steer clear of fatty foods. If shortness of breath becomes an issue due to pressure on your diaphragm, good posture can help, and relief often comes when the baby moves lower into the pelvis. After the first trimester, it’s best to sleep on your left side to reduce pressure on major blood vessels and encourage better blood flow to your baby.
Conclusion
Your hormones play an incredible role in transforming your uterus from a small, fist-sized organ into a supportive environment for your growing baby. These hormones work in a carefully timed sequence to create a safe and adaptable space for pregnancy. Estrogen promotes growth, boosting blood flow and preparing the uterus to accommodate a full-term baby. Meanwhile, Relaxin softens the cervix and loosens pelvic ligaments, ensuring your body is physically ready for both pregnancy and delivery.
Knowing how these hormonal changes affect you can make it easier to manage symptoms and recognize when to seek medical advice. For instance, understanding that progesterone relaxes digestive muscles and causes heartburn, or that swelling comes from increased blood volume, helps you address these shifts more effectively. As Hearth and Home Midwifery explains:
"When you understand what your body is doing, it's easier to trust it through the process."
These hormones don’t act alone - they work together in what researchers describe as a "collective event of molecular, physiological, and anatomical adaptations." Every symptom you experience reflects your body’s intricate response to pregnancy, showing just how well it knows what to do.
To support these processes, stay consistent with prenatal care. Regular checkups ensure that your uterine growth, blood flow, and overall health remain on track. If symptoms become overwhelming or you experience concerning signs like extreme swelling or severe headaches, don’t hesitate to reach out to your healthcare provider for guidance.
FAQs
What can cause hCG levels to rise more slowly than expected?
HCG levels can sometimes increase at a slower rate than anticipated. This may point to concerns such as an abnormal pregnancy or a higher likelihood of miscarriage. While the exact reasons for this aren't outlined here, it's crucial to address any questions or worries about hCG levels with your healthcare provider. They can offer a thorough evaluation and the guidance you need.
How do doctors tell normal uterine stretching from preterm labor?
Doctors distinguish between normal uterine stretching and preterm labor by combining clinical evaluations, patient history, and diagnostic tools. Normal uterine stretching typically causes gradual, painless growth as the uterus expands to accommodate the baby. In contrast, preterm labor is marked by painful, consistent contractions and changes in the cervix that occur before 37 weeks of pregnancy.
To identify preterm labor, doctors watch for symptoms like persistent back pain, increased pelvic pressure, or cervical dilation. Diagnostic tools such as ultrasounds and specific lab tests are often used to confirm whether labor is beginning too early. These assessments help ensure timely and accurate care.
When should swelling or headaches be treated as an urgent warning sign?
If you experience severe or persistent swelling or headaches, especially when accompanied by symptoms like vision changes or high blood pressure, it could indicate serious conditions such as preeclampsia. These situations require immediate medical attention. Be sure to contact your healthcare provider right away if you notice these symptoms.
The views, statements, and pricing expressed are deemed reliable as of the published date. Articles may not reflect current pricing, offerings, or recent innovations.