Why Stem Cell Yield Matters: The Science Behind Americord’s Method
Placental tissue is emerging as a powerful resource in regenerative medicine, offering unique benefits alongside cord blood. While cord blood is widely known for its use in treating blood and immune system disorders, placental tissue provides a rich source of Mesenchymal Stem Cells (MSCs) and growth factors that aid in repairing and regenerating tissues like bone, cartilage, muscle, and skin. Here’s why it matters:
- Cell Types: Placental tissue contains MSCs and Human Amniotic Epithelial Cells (hAECs), which promote tissue repair and reduce inflammation.
- Immune-Privileged: Lower rejection risk makes it suitable for broader use, including unrelated patients.
- Volume Advantage: A single placenta can yield up to 7,000 doses of MSCs, far exceeding the capacity of cord blood.
- Applications: Currently used in wound healing, orthopedic repair, and neurological research, with over 300 clinical trials underway.
- Storage: Processed and preserved in liquid nitrogen, placental tissue remains viable for decades.
Banking both cord blood and placental tissue ensures families have access to complementary treatments for a wide range of medical needs.
What Makes Placental Tissue Different?
Placental tissue takes cord blood banking a step further, offering unique regenerative benefits thanks to its diverse cellular and molecular properties. While cord blood is a rich source of Hematopoietic Stem Cells (HSCs) used in blood and immune system therapies, placental tissue stands out with its Mesenchymal Stem Cells (MSCs) and a variety of growth factors that aid in tissue repair and regeneration.
Cell Types and Growth Factors
The placenta is home to several types of stem cells, including Human Amniotic Epithelial Cells (hAECs) and MSCs found in the amnion, chorion, and chorionic villi. These cells express embryonic markers like Oct-4, Nanog, and Sox-2, giving them high pluripotency without the ethical concerns or tumor risks associated with embryonic stem cells.
Placental tissue also contains key proteins such as VEGF (vascular endothelial growth factor), EGF (epithelial growth factor), and FGFs (fibroblast growth factors). These molecules play vital roles in promoting blood vessel growth, reducing inflammation, speeding up wound healing, and producing antimicrobial peptides like defensins to prevent infections.
"Placental tissues are of great interest in medicine, specifically as a biomaterial because of the exceptional properties of fetal tissues and the ease of access to them as raw materials." - Annelise Roy, Research and Development, StimLabs LLC
Another standout feature is the tissue’s immune-privileged status, characterized by low levels of MHC class II molecules and HLA-G. This makes it suitable for allogeneic transplants, reducing the risk of rejection and allowing it to potentially benefit both family members and unrelated patients.
Volume and Quantity
One of the challenges with cord blood is its limited volume, which often falls short for treating adults or offering multiple rounds of therapy. Placental tissue addresses this issue by serving as a much larger reservoir of stem cells and biological materials.
A single full-term placenta, with an average surface area of 1,600 cm², can produce between 80–300 million hAECs and 20–50 million MSCs. This means one placenta has the potential to generate up to 7,000 clinical doses of MSCs, far surpassing the single-use limitations of cord blood.
Studies have shown that placental MSCs have greater clonogenic ability than those derived from cord blood, meaning they can form more colonies and expand more effectively for clinical use. In fact, placental MSCs have been found to be 2.1 times more effective in reducing T-cell proliferation compared to cord-derived MSCs, highlighting their stronger immunosuppressive capabilities. This abundance of cells opens the door to a wide range of therapeutic applications.
Processing and Long-Term Storage
To ensure optimal cell viability, placental tissue must be processed within 6 hours of birth. The placenta is collected aseptically during delivery and transported in sterile containers, either at room temperature or cooled to 39°F (4°C). The processing involves several precise steps: the placenta is divided into regions (decidua, chorionic plate, and chorionic villi), cut into small pieces (1–5 mm³), and incubated for 1–2 hours at 98.6°F (37°C) in a solution containing collagenase type I, DNase I, and dispase. Mononuclear cells are then separated using pulse centrifugation and filtered through a 100 µm mesh to remove clumps.
For long-term preservation, cells are treated with cryoprotectants like Dimethyl sulfoxide (DMSO) and frozen using a controlled-rate process. The materials are stored in vapor-phase liquid nitrogen, which allows them to remain viable for decades. This meticulous preservation process ensures the tissue is ready for future medical use whenever needed.
How Placental Tissue Compares to Cord Blood
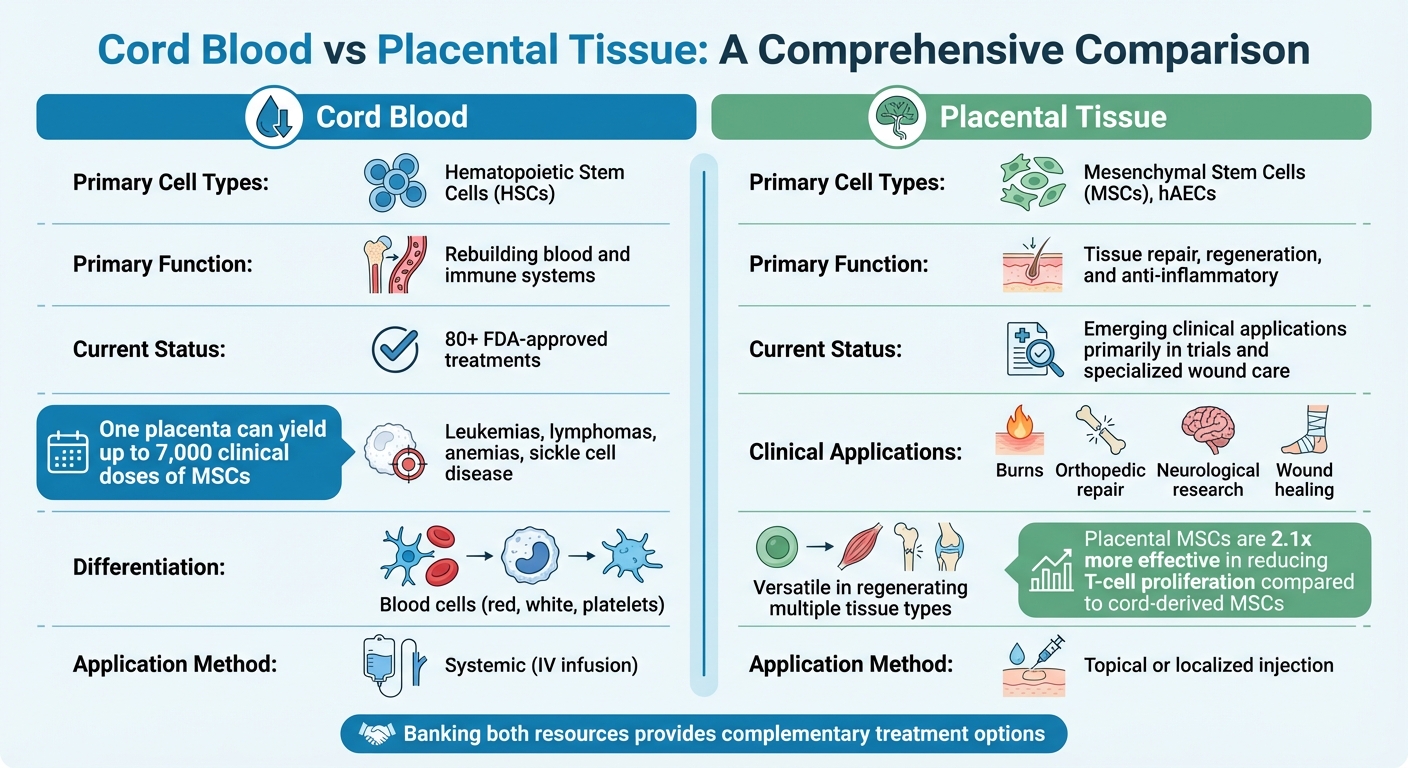
Cord Blood vs Placental Tissue: Key Differences in Stem Cell Banking
Cord blood and placental tissue complement each other, offering families a broader range of medical possibilities. Each resource has unique strengths: cord blood excels in rebuilding blood and immune systems with Hematopoietic Stem Cells (HSCs), while placental tissue focuses on tissue repair and regeneration through Mesenchymal Stem Cells (MSCs) and growth factors.
Side-by-Side Comparison
Here's a closer look at how these two resources differ and what they bring to the table:
| Feature | Cord Blood | Placental Tissue |
|---|---|---|
| Primary Cell Types | Hematopoietic Stem Cells (HSCs) | Mesenchymal Stem Cells (MSCs), hAECs |
| Primary Function | Rebuilding blood and immune systems | Tissue repair, regeneration, and anti-inflammatory |
| Current Status | 80+ FDA-approved treatments | Emerging clinical applications primarily in trials and specialized wound care |
| Clinical Applications | Leukemias, lymphomas, anemias, sickle cell disease | Burns, orthopedic repair, neurological research, wound healing |
| Differentiation | Blood cells (red, white, platelets) | Versatile in regenerating multiple tissue types |
| Application Method | Systemic (IV infusion) | Topical or localized injection |
Cord blood has a well-established role in treating over 80 medical conditions, thanks to its FDA-approved applications. On the other hand, placental tissue is carving out its niche in areas like wound care, orthopedic repairs, and neurological research. While cord blood is ideal for systemic disorders, placental tissue offers exciting possibilities for localized and regenerative therapies.
Expanded Treatment Options
Placental tissue doesn't just complement cord blood - it opens doors to therapies that cord blood alone cannot address. MSCs from placental tissue can transform into bone, cartilage, muscle, and even nerve cells, making them a valuable asset for various conditions. This includes orthopedic repairs like tendinitis and plantar fasciitis, neurological conditions such as Alzheimer's and Parkinson's disease, and surgical applications where it helps reduce scarring and adhesions.
"The multiple-lineage differentiation potential of placental MSCs presents an invaluable future for clinical applications." - Wang Y and Zhao S, Vascular Biology of the Placenta
Research also shows that placental MSCs can expand cord blood HSCs outside the body, boosting the effectiveness of cellular therapies for patients of all ages. Together, cord blood and placental tissue create a comprehensive treatment landscape: cord blood tackles systemic blood-related disorders, while placental tissue focuses on localized repair and reducing inflammation.
Banking both resources at the same time ensures families are prepared for a wide range of future medical treatments. This dual-resource approach not only maximizes therapeutic options but also offers a cost-efficient way to secure these benefits through a single donor screening process. By combining the strengths of both cord blood and placental tissue, families can access a more versatile and complete set of treatment possibilities.
Medical Uses Today and Tomorrow
Placental tissue is making waves in modern medicine, with over 50 ongoing studies investigating its role in areas like wound care, neurological recovery, and orthopedic repair. Here’s a closer look at how this tissue is reshaping treatment approaches.
Wound Healing and Burn Treatment
Chronic wounds impact 8.2 million Medicare patients in the U.S., costing up to $96.8 billion annually. Placental tissue grafts offer a powerful solution thanks to their natural antimicrobial, anti-inflammatory, and tissue-remodeling properties. Acting as a biological scaffold, the placental membrane supports cell migration and growth, creating the perfect conditions for healing.
For example, placental tissue grafts have shown over 98% healing success in diabetic foot ulcers within just six weeks. In burn care, the results are equally compelling - a patient with severe facial burns experienced complete tissue regeneration within weeks after treatment with placental tissue.
Currently, these grafts are used for conditions like diabetic foot ulcers, venous stasis ulcers, pressure sores, partial-thickness burns, and surgical wounds.
Orthopedic and Joint Repair
Placental tissue is also gaining traction in orthopedics, offering less invasive options for conditions that typically require surgery or lengthy recovery periods. Packed with mesenchymal stromal cells (MSCs) and growth factors, it helps reduce inflammation and speeds up the repair process in joints, tendons, and ligaments. Doctors are using it to treat knee osteoarthritis, tendinitis, ligament sprains, and plantar fasciitis. Depending on the injury, the tissue can be applied directly or injected to deliver its regenerative benefits right where they’re needed.
One of its most exciting uses is in cartilage repair, an area where healing is notoriously slow. The tissue’s extracellular matrix acts as a scaffold for new growth, while its anti-inflammatory properties create an environment conducive to long-term recovery.
Research in Neurological Conditions
Neurological applications of placental tissue are still in early stages, but the potential is enormous. Human amniotic mesenchymal stromal cells (hAMSCs) derived from placental tissue are being studied for their ability to transform into neuroglial cells and aid recovery in the central nervous system. Research from 2023 revealed that hAMSCs can stimulate axon growth in damaged neurons, a critical step in restoring function. These cells also appear to reduce brain inflammation and cell death, suggesting possible treatments for conditions like ischemic stroke, Parkinson’s disease, and spinal cord injuries.
Clinical trials are now exploring placental tissue derivatives for autism, cerebral palsy, multiple sclerosis, and stroke recovery, opening the door to transformative therapies in neurology.
Banking Placental Tissue with Americord Registry
With the growing potential of placental tissue in clinical treatments, securely banking it has become increasingly important.
Family Plan Options
Americord Registry provides a range of family preservation plans that include placental tissue banking. The Complete Family Plan combines cord blood, cord tissue, and placental tissue banking into one package. This ensures families have access to a variety of stem cell types: blood-forming stem cells from cord blood, as well as mesenchymal stem cells and growth factors found in the placental membrane.
For those seeking a more extensive option, the Ultimate Family Plan adds newborn exosome banking to the mix, along with enhanced CryoMaxx™ processing to maximize cell viability. This plan offers families access to a broader range of regenerative medicine possibilities as new therapies are developed. The collection process takes place right after delivery and does not interfere with delayed cord clamping or the birthing experience. Americord’s advanced methods ensure a seamless and effective preservation process.
CryoMaxx™ Processing and Storage
Americord’s CryoMaxx™ technology uses a precise, minimal manipulation approach to isolate the amnion and chorion layers of the placental membrane. This process preserves the multipotent cells, growth factors, and cytokines naturally present in the tissue. Manual processing allows for strict quality control.
Once processed, the placental tissue is stored in multiple vials at an ultra-low temperature of –196°C in liquid nitrogen. These FDA-registered, AABB-accredited facilities ensure long-term preservation. The segmented storage system means families can access portions of the tissue for different uses, such as wound care, orthopedic treatments, or participation in clinical trials. Research indicates that properly banked cells could remain viable for over 200 years. Americord’s meticulous processing ensures the tissue’s quality and usability for future applications.
Quality Standards and Customer Support
Americord adheres to high standards, with accreditations from AABB and FACT. They back their services with a $110,000 Cord Blood Quality Guarantee, which covers the cost of finding an alternative stem cell source if the banked cord blood does not engraft.
The pricing is straightforward, with initial collection costs ranging between $3,000 and $5,000, depending on the chosen plan, and annual storage fees of around $200. Families are only billed for processing and storage after the baby’s birth. Americord also provides 24/7 customer support, free genetic counseling, and dedicated account managers to make the enrollment process smooth and customizable to each family’s needs.
The Future of Placental Tissue in Medicine
New Clinical Trials
Research into the medical uses of placental tissue is gaining momentum. In the U.S. alone, over 2,000 clinical trials are currently exploring perinatal stem cells, with placental tissue playing a key role.
Among the most promising areas of study are human amnion epithelial cells (hAECs), which are being closely examined due to their regenerative abilities and immune-friendly nature. Placental tissue also provides a rich source of mesenchymal stromal cells (MSCs). In fact, a single full-term placenta can yield almost 500 million hAMSCs without requiring additional lab expansion. As of 2023, hAECs are being tested in clinical trials for conditions like end-stage liver diseases (trial registry ACTRN 12616000437460) and Crohn's disease-related perianal fistulas (trial registry ACTRN 12618001883202). Preclinical studies have also shown encouraging results - rats with spinal cord injuries treated with placental MSCs experienced noticeable improvements in sensory response and walking ability compared to untreated groups.
Another exciting development involves cell-free therapies that utilize extracellular vesicles and exosomes derived from placental cells. These methods aim to deliver regenerative benefits without the potential risks tied to live cell transplants. Additionally, researchers are investigating the placenta's extracellular matrix as a bioactive scaffold for tissue engineering. This could lead to advancements in creating artificial implants and disease models.
These breakthroughs highlight the growing potential of placental tissue in shaping future medical treatments.
A Health Resource for the Future
As medical research progresses, the importance of placental tissue becomes even more apparent. Banking this tissue ensures access to therapies that might only become available years down the road. Since standard 20-year storage plans may expire before such treatments are fully developed, many families are now considering lifetime storage options.
"The placenta obtained from full term delivery is a good source of tissue suitable for obtaining good quality MSCs in large numbers... it could serve as a gold mine for translational/clinical research." – Reproductive Biology Journal
The range of possible applications continues to grow, with ongoing studies focusing on treatments for neurological, autoimmune, cardiovascular, and metabolic conditions. Given that regenerative medicine could benefit one in three people, storing placental tissue is increasingly seen as a forward-thinking health investment for families.
Conclusion
The field of clinical research is advancing quickly, turning scientific progress into practical health solutions for families. Placental tissue has emerged as a key player in regenerative medicine, offering families a range of regenerative elements that, when combined with cord blood, open the door to expanded treatment possibilities. With over 2,000 clinical trials currently focused on perinatal stem cells, banking placental tissue is increasingly becoming a forward-looking health choice for parents.
Placental tissue stands out due to its unique features: its thin structure supports specialized wound healing, its immune-privileged status allows for broader family use, and it enhances the effectiveness of cord blood transplants. Placental mesenchymal stem cells (MSCs) also increase hematopoietic cell counts, addressing the volume limitations of cord blood.
Americord Registry offers comprehensive options like the Complete and Ultimate Family Plans, which include cord blood, cord tissue, and placental tissue banking. With CryoMaxx™ processing, these services are available for approximately $2,000 at collection and $150 annually.
As clinical trials continue to explore treatments for conditions like autism, cerebral palsy, type 2 diabetes, and heart failure, banking placental tissue today could provide access to therapies that may take years to become widely available. Early enrollment ensures the timely arrival of collection kits, even in cases of premature birth.
Choosing to bank placental tissue with Americord Registry is an investment in your family’s health and future treatment opportunities.
FAQs
Can my baby’s banked placental tissue be used for parents or siblings?
Yes, the placental tissue you’ve banked for your baby might also be useful for parents or siblings. This tissue is rich in stem cells, which could play a role in regenerative treatments, provided there’s a match and it aligns with the medical requirements of the family member in need.
What’s the difference between placental tissue and cord tissue?
Placental tissue is unique because it holds both fetal and maternal stem cells, creating a blend of regenerative qualities. On the other hand, cord tissue is primarily made up of fetal mesenchymal stem cells, which are located in the umbilical cord.
How often are banked placental cells used in treatments today?
Placental cells stored in banks are primarily utilized for wound healing and regenerative treatments. These applications have been documented in cases like burns, ulcers, and surgical wounds.
The views, statements, and pricing expressed are deemed reliable as of the published date. Articles may not reflect current pricing, offerings, or recent innovations.