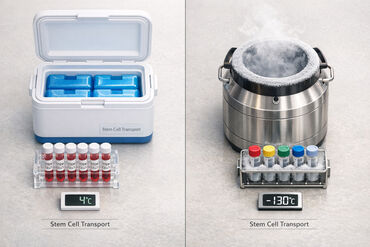
Why Temperature Control Matters for Cord Blood
Proper temperature control is critical for preserving the viability of cord blood stem cells, which are used to treat nearly 80 diseases and hold potential for emerging therapies. Without maintaining the recommended temperature range during transport (39°F to 86°F or stricter ranges), stem cells can suffer irreversible damage, compromising their ability to support life-saving treatments. Regulatory guidelines and advanced transport systems ensure these cells remain functional, safeguarding their long-term medical use.
Key takeaways:
- Temperature sensitivity: Stem cells are highly vulnerable to heat and cold, which can cause cell death or structural damage.
- Transport standards: Safe ranges (4°C–30°C or stricter) are enforced by organizations like the FDA and FACT to maintain cell viability.
- Long-term storage: Proper cryopreservation at -320°F ensures cells remain viable for decades, with studies showing 92%+ viability even after 23 years.
Maintaining strict temperature control from collection to storage ensures these cells retain their life-saving potential for future medical treatments.
Why Cord Blood Stem Cells Are Sensitive to Temperature
Preserving the life-saving potential of cord blood hinges on understanding why its stem cells are so sensitive to temperature changes. These cells need a stable environment to retain their structure and function, and extreme conditions can jeopardize their viability.
The biological makeup of cord blood stem cells makes them especially vulnerable to "temperature excursions" - any deviation from safe temperature ranges. These excursions often occur during transport, such as when packages are shipped in unconditioned cargo holds or delayed between collection and laboratory arrival. Each of these scenarios increases the risk of damage to the cells.
Thermal stress interferes with cellular processes and can lead to cell death, which is why regulatory bodies like the FDA, AABB, and FACT enforce strict guidelines to ensure careful temperature control during transport.
The Recommended Temperature Range for Transport
To protect cord blood stem cells during transport, regulatory authorities advise keeping fresh cord blood within a temperature range of 4°C to 30°C (39°F to 86°F). However, many cord blood banks adopt a stricter range of 2°C to 8°C (36°F to 46°F) for added safety. This narrower range helps mitigate the inevitable fluctuations that can happen during shipping.
Since July 2013, the Foundation for the Accreditation of Cellular Therapy (FACT) has required family bank kits to include temperature monitoring tools. This ensures that any deviations from the safe range during shipment are recorded. Such measures underscore how vital it is to maintain precise temperature control, as exceeding these limits can cause immediate and irreversible damage to the cells.
What Happens When Temperature Goes Outside the Safe Range
When cord blood is exposed to temperatures outside the recommended range, cell damage occurs quickly. Heat speeds up cellular metabolism, often leading to cell death, while extreme cold can cause ice crystals to form, which rupture cell membranes. Both conditions severely compromise the cells' viability and their therapeutic potential.
Security regulations introduced after 2001 have added new challenges. Medical couriers are no longer allowed to hand-carry cord blood units into temperature-controlled airplane cabins. Instead, these units must travel in cargo holds, where temperature control relies entirely on the insulation of the cord blood collection kit. Delays or cancellations can leave the cells exposed to extreme temperatures for hours, potentially rendering them unusable before they even reach the lab.
How Temperature Problems Damage Cord Blood
Cell Damage from Extreme Temperatures
Cord blood stem cells are highly sensitive to temperature changes, and exposure to extreme heat or cold can cause irreversible harm. Excessive heat accelerates the cells' metabolism, overwhelming their natural processes and leading to cell death. This is particularly damaging to granulocyte-monocyte precursors and other progenitor cells, which are critical for forming blood and immune systems.
On the other hand, extreme cold can also wreak havoc. When cord blood is exposed to temperatures that are too low during transport, the cells may suffer structural damage. This kind of harm happens quickly and cannot be undone, leaving the cells unable to function properly.
Both types of temperature stress reduce the cells' ability to multiply and perform their vital roles. Even if some cells survive, their functionality may be compromised, which can severely impact their effectiveness in future medical treatments.
Effects on Future Medical Treatments
The damage caused by temperature issues doesn't just affect the cells - it directly impacts their ability to support critical medical treatments. Cord blood stem cells play a key role in hematopoietic reconstitution, a process where transplanted cells rebuild a patient’s blood and immune system. If the cells are damaged, they may fail to perform this essential task, increasing the likelihood of transplant failure.
Cryo-Cell International conducted stability testing in March 2020, led by Laboratory Director Todd Schuesler, on cord blood samples stored since 1996. The results were impressive: after 23.5 years of proper cryogenic storage, the CD34+ viability of the cells remained at 92% or higher. This demonstrates that maintaining the correct temperature ensures the long-term viability of stem cells, potentially for the donor’s entire lifetime. However, cells exposed to temperature fluctuations during transport can lose viability quickly, rendering them unsuitable for medical use.
Cord blood is FDA-approved to treat over 80 FDA-approved treatments for diseases affecting the blood and immune system. If temperature issues compromise the cells before they reach long-term storage, their therapeutic potential is lost, and with it, the chance to provide life-saving treatments.
Methods for Maintaining Proper Temperature Control
Specialized Transport Systems
Transporting cord blood safely requires more than just tossing it into a basic cooler. Insulated shipping kits are the cornerstone of temperature control. These kits are designed to protect stem cells from extreme temperatures - whether it's a blazing hot summer day or subzero conditions in a cargo hold. Their robust construction ensures the cells remain safe throughout the journey.
The Foundation for the Accreditation of Cellular Therapy (FACT) has strict guidelines for monitoring transport conditions. According to their standards, "Standard C7.5.2 requires that the temperature inside the outer container be continuously monitored." To meet these requirements, quality shipping kits often include temperature loggers that track conditions during transit or detectors that alert if the internal temperature strays outside the safe range of 39°F to 86°F (4°C to 30°C).
Specialized medical courier services are essential for transporting cord blood. Unlike standard shipping options, these couriers use temperature-controlled vehicles and ensure a secure chain of custody from the hospital to the lab. They deliver the cord blood directly to lab personnel, avoiding the risks of uncontrolled environments. This role became even more critical after 9/11, when new regulations prevented couriers from hand-carrying kits onto planes. As a result, the reliability of insulated kits and their monitoring systems became even more important.
High-quality transport systems are rigorously tested by third-party organizations like the International Safe Transit Association (ISTA) and the International Air Transport Association (IATA). These tests simulate extreme heat and cold conditions to confirm the kits perform as needed in real-world scenarios. Public cord blood banks often require these kits to maintain stable temperatures for up to 48 hours, while private banks, relying on faster courier deliveries, typically use smaller, more compact kits.
Once the cord blood arrives safely at the lab, maintaining proper temperature continues to be a priority as it moves into the cryopreservation stage.
Long-Term Storage Methods
After transport, the focus shifts to cryopreservation, a highly specialized process that freezes cells at ultra-low temperatures for long-term storage. This isn’t as simple as sticking samples in a freezer. The process involves preparing the cells with cryoprotectants and cooling them at controlled rates to avoid ice crystal formation, which could damage cell membranes.
Cryopreservation techniques are designed to preserve the viability of stem cells for future medical use. Storage takes place in cryogenic tanks that maintain temperatures around -320°F (-196°C) using liquid nitrogen. Many modern facilities use 5-compartment storage vials, which allow a single cord blood unit to be divided for multiple treatments. Additionally, these tanks are equipped with continuous monitoring systems that track temperatures around the clock to ensure stability is never compromised.
How Americord Registry Maintains Temperature Stability
CryoMaxx™ Processing for Cell Viability
Americord Registry relies on CryoMaxx™ Processing, a specialized method designed to prioritize temperature control at every stage. This technique minimizes handling to preserve stem cells, ensuring they remain viable for future use. The entire process happens in pharmaceutical-grade clean rooms located in New Jersey.
Even before processing begins, samples are protected during transit using advanced shipping containers. These containers are rigorously tested to withstand extreme temperatures, safeguarding the cord blood from the moment it leaves the hospital, regardless of weather conditions. This is a critical step in how the collection process works to ensure sample integrity.
After processing, tissues are stored in the vapor phase of cryogenic freezers at temperatures as low as -320°F (-196°C). This method avoids direct contact with liquid nitrogen while maintaining the ultra-cold environment required for preservation. Americord backs this system with their $110,000 engraftment guarantee10,000 engraftment guarantee, the highest in the industry, which covers the cost of an alternative stem cell source if stored cells fail to engraft during a transplant.
This seamless process transitions cord blood into secure, long-term storage, supported by strict protocols to ensure the safety and reliability of every sample.
AABB-Accredited Storage Systems
Americord’s storage facilities meet the stringent standards set by the AABB (Association for the Advancement of Blood & Biotherapies). This accreditation confirms that the facility consistently follows rigorous procedures for collecting, processing, and storing cord blood. It’s not just a formality - it’s evidence of their commitment to reliability and maintaining temperature stability throughout the storage lifecycle.
Their systems include 24/7 continuous monitoring with automatic alerts to notify staff immediately if any temperature deviations occur. This constant oversight ensures that samples remain at stable cryogenic temperatures without interruption. Using 5-compartment storage vials alongside separate cryovials, Americord provides secure and flexible options for long-term preservation. Their protocols have proven effective, with a 100% success rate for the 14 cord blood units they’ve released for autologous transplants.
These combined measures ensure that stem cells are preserved under optimal conditions, safeguarding their life-saving potential for the future.
Conclusion
Maintaining proper temperature control is absolutely essential for keeping cord blood stem cells viable. From the moment of collection to long-term cryopreservation, ensuring stable temperatures - between 39°F and 86°F (4°C and 30°C) during transport and at cryogenic levels of -320°F (-196°C) for storage - helps prevent irreversible damage to the cells.
In the summer of 2023, research led by Dr. Hal Broxmeyer's team revealed that cord blood, cryopreserved for 27 years, remained viable. Similarly, in May 2023, a young adult in China was successfully treated for aplastic anemia using their own cord blood, which had been stored for 19 years. These real-world examples highlight the importance of strict temperature control in cord blood banking.
Americord Registry ensures reliable temperature stability through its CryoMaxx™ Processing, AABB-accredited facilities, and around-the-clock monitoring. By choosing a cord blood bank with these high standards, you're making an investment in your family's health and future, backed by a commitment to excellence at every stage.
FAQs
How can parents tell if a cord blood kit stayed in the safe temperature range during shipping?
Parents can confirm whether a cord blood kit stayed within the safe temperature range by reviewing the temperature indicators or data loggers included with the kit. These tools track and document any temperature fluctuations during transit, ensuring the kit was kept under proper conditions.
What happens if cord blood is delayed in transit or exposed to cargo-hold temperatures?
Proper transportation of cord blood is essential to maintain the viability of stem cells. If the cord blood faces delays or is subjected to extreme temperatures - whether too hot or too cold - during transit, the stem cells may lose their effectiveness. This could impact their potential use in future medical treatments. Ensuring stable, controlled temperatures throughout transport is key to preserving the quality of these cells.
How does vapor-phase liquid nitrogen storage keep cord blood viable for decades?
Vapor-phase liquid nitrogen storage is an effective method for preserving cord blood for decades. By maintaining a temperature of around −190°C, this process halts all cellular activity. This extreme cold prevents any degradation, ensuring that stem cells stay viable for long-term use. Maintaining precise temperature control is crucial to protect the quality and usability of these stored stem cells.
The views, statements, and pricing expressed are deemed reliable as of the published date. Articles may not reflect current pricing, offerings, or recent innovations.